
CVS Health Case Study: Digital Transformation & Agentic AI Strategy 2026
Strategic Overview
CVS Health enters 2026 operating across 185 million annual consumer touchpoints and $372.8B in FY2024 revenue — and has made a decisive architectural bet that will define its next decade: platform consolidation over unit-level optimization, collapsing three autonomous businesses into a single AI-native consumer engagement layer. The mechanism is an agentic AI infrastructure — including Agentic Twins, Google Cloud/Gemini integration, and a unified consumer app — that harmonizes clinical and transactional data across the payer-PBM-pharmacy boundary for the first time. Early results validate the thesis: integrated members show a 3–6% decrease in per-member-per-month medical costs, 97% of CVS Specialty patients prefer digital CareTeam engagement, and mid-teens adjusted EPS growth is projected through 2028. The stakes extend beyond operational efficiency — CVS is constructing a proprietary behavioral data asset designed to make it structurally indispensable to employers, payers, and the broader U.S. healthcare ecosystem.
Let’s kickstart the conversation and design stuff people will love.

CVS Health Digital Transformation: From Fragmented Enterprise to Unified Health Platform
CVS Health enters 2026 as the largest healthcare company in the United States by revenue, generating $372.8 billion in FY2024, with Q1 2025 revenue of $94.6 billion already signaling an upward trajectory toward its $400 billion full-year guidance. Scale, however, has historically been CVS's structural liability as much as its competitive advantage. The 2018 Aetna acquisition added a $69 billion payer to a pharmacy and PBM enterprise, creating the theoretical conditions for integrated care, but also three distinct business unit cultures, three separate technology architectures, and three regulatory environments operating under one corporate umbrella.
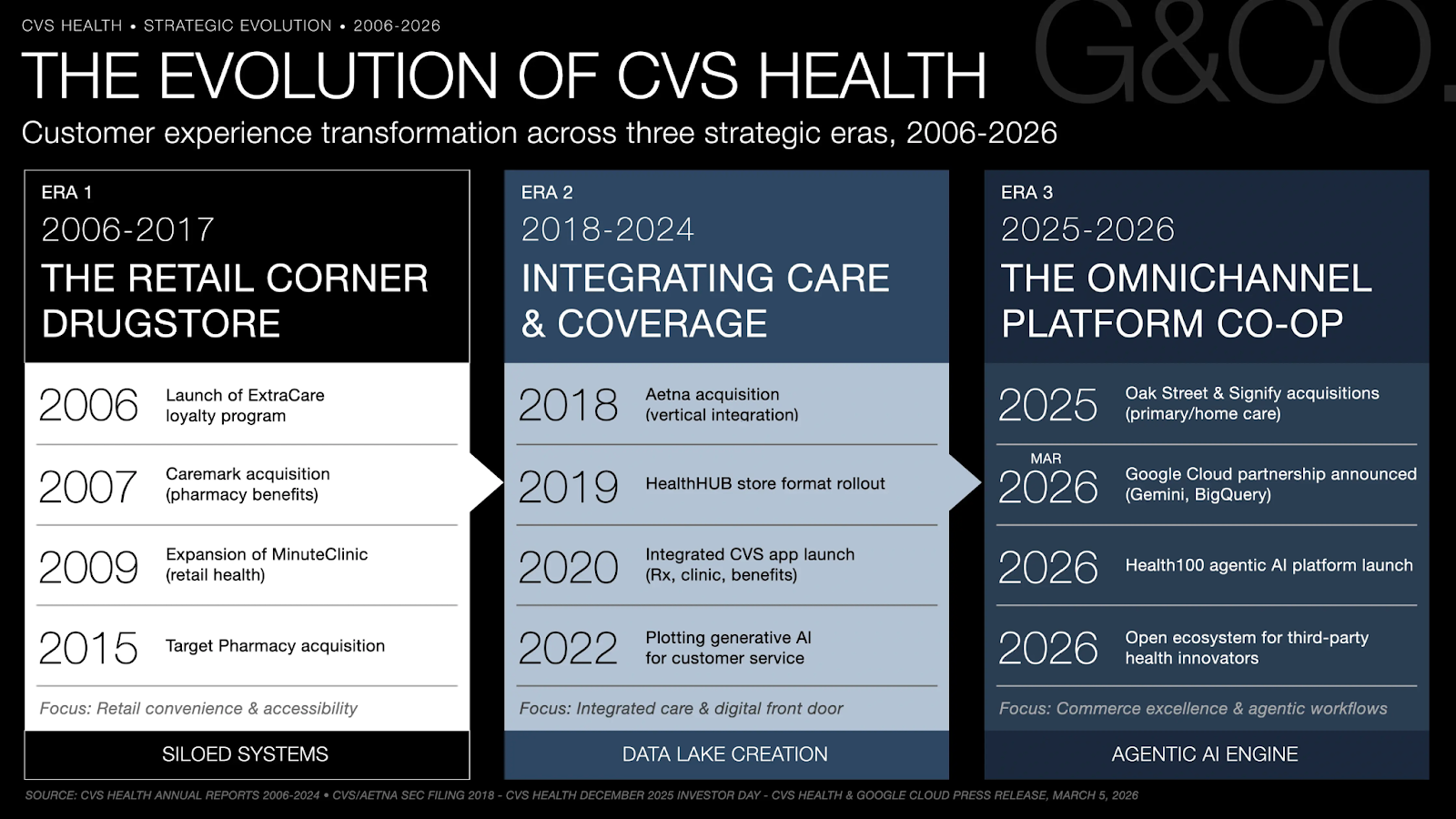
The "Moment of Inertia" driving the current strategy is not technological lag, it is identity fragmentation. A CVS Pharmacy customer, a Caremark PBM member, and an Aetna plan participant could be the same individual navigating three separate digital interfaces, receiving three uncoordinated communications, and generating three disconnected data trails. That fragmentation is not merely a user experience failure. It is a structural inefficiency that prevents CVS from deploying its most valuable asset: the longitudinal behavioral and clinical data that flows across all three units when unified. Healthcare digital transformation at CVS is therefore less about digitizing existing processes and more about constructing the connective infrastructure that makes integration commercially viable for the first time.
The Strategic Choice: Platform Over Product
CVS leadership made a decisive architectural choice between 2023 and 2025: prioritize platform consolidation over point-solution optimization. The alternative path, incrementally improving each business unit's digital interface independently, would have produced faster short-term wins but permanently foreclosed the integrated data layer that underpins the long-term strategy. CEO David Joyner articulated the frame at the December 2025 Investor Day: healthcare today is fragmented and difficult to navigate, and CVS's competitive position depends on creating a simpler, more connected experience with technology at its center.
The trade-off this choice mandated is significant. CVS Health AI strategy resources that could have been deployed to accelerate Aetna's Medicare Advantage recovery, under severe margin pressure in 2023–2024, were instead directed toward infrastructure that produces no immediate revenue. Caremark's PBM operations, which generate the highest margin contribution of the three units, were subordinated to an integration roadmap that prioritizes consumer experience coherence over business unit autonomy. Leadership explicitly chose to absorb short-term earnings pressure to preserve the integrity of the platform architecture, a conviction that the "Engagement as a Service" model represents a category-defining revenue stream unavailable to any competitor without equivalent scale.
From Strategy to Execution: The Plumbing of Agentic AI in Healthcare
The execution of CVS Health's omnichannel strategy operates across four distinct but interdependent infrastructure layers. The first is the Unified CVS Health App, launched in January 2025, which replaced the legacy CVS Pharmacy application with an all-in-one platform managing prescriptions across CVS Pharmacy, Caremark mail-order, and CVS Specialty, integrating immunization scheduling, AI-powered medication search, health spending visibility, and personalized health reminders into a single authenticated consumer session. For the first time, a Caremark member and a CVS Pharmacy patient share the same digital front door.
The second layer is the agentic AI infrastructure powering the platform's intelligence. CVS's partnership with Google Cloud deploys Gemini multimodal models for proactive patient engagement, with Cloud Healthcare API and BigQuery harmonizing clinical and transactional data across business units. This is the data architecture that makes the consumer layer commercially viable, without it, personalization is cosmetic. The third layer is the Agentic Twins capability, AI-powered synthetic patient models built from consented behavioral data across hundreds of thousands of individuals. These digital personas allow product and clinical teams to pressure-test digital workflows against simulated real-patient behavior, compressing research cycles from weeks to hours and eliminating the need to deploy untested features to live populations.
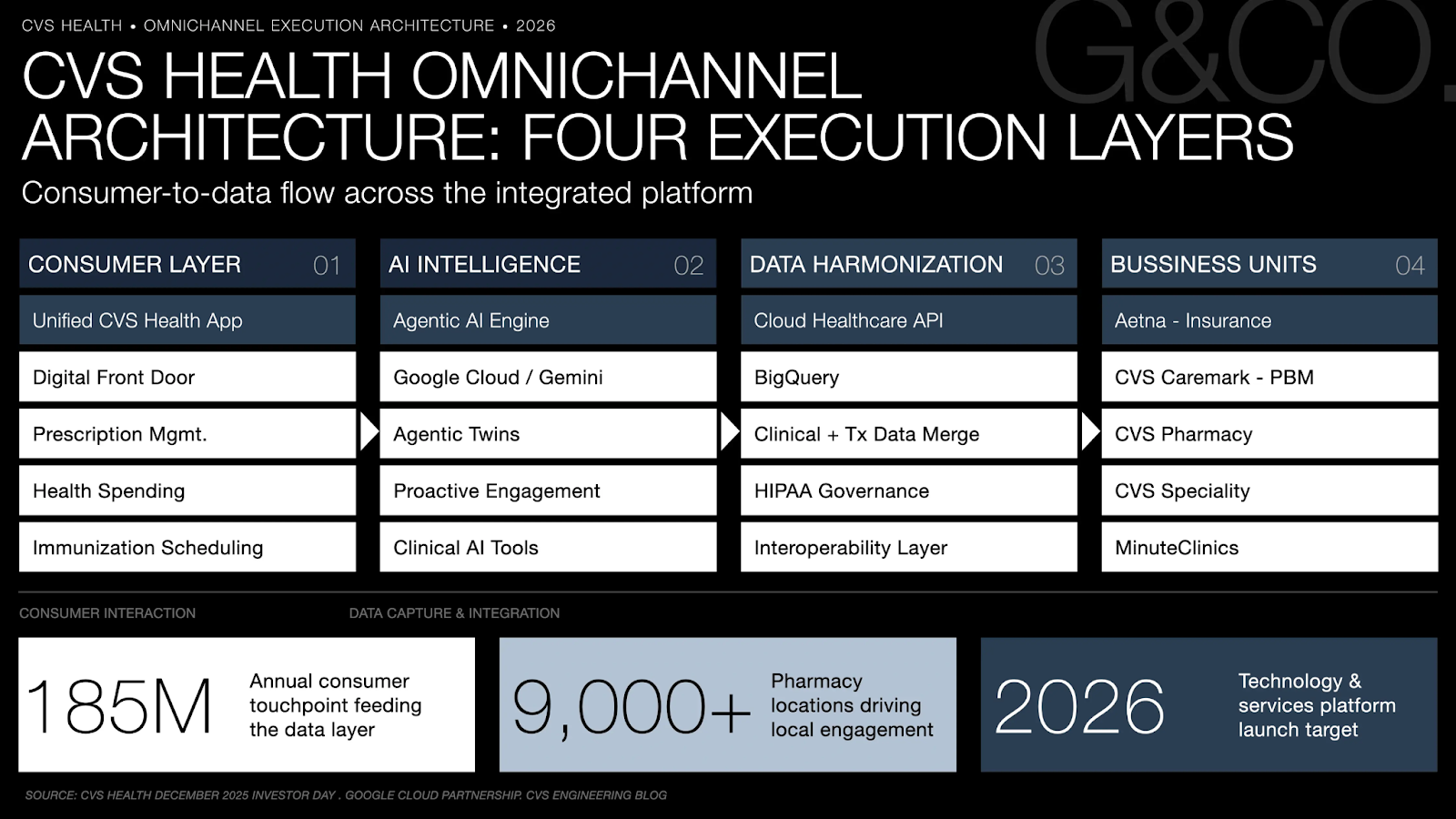
The fourth layer, the least visible externally, is the clinician-facing AI tooling that closes the loop between consumer engagement and care delivery. CVS Specialty pharmacy patients interact with AI-supported CareTeams via two-way secure messaging; clinicians use AI-generated case note summaries to redirect time toward clinical judgment rather than documentation. This layer is critical to the customer journey case study because it demonstrates that CVS's omnichannel architecture does not terminate at the consumer interface, it extends into the clinical workflow, creating a continuous engagement loop that generates additional behavioral data at every interaction point.
The Strategy–Execution Gap: Where Intent Meets Institutional Friction
The structural tension in CVS's transformation is not technological, it is organizational. Three business units that operated as autonomous enterprises for years, each with distinct P&L accountability, talent cultures, and vendor relationships, are being asked to subordinate unit-level optimization to a platform logic that distributes benefits unevenly and on a multi-year timeline. The AI in healthcare case study literature consistently identifies this pattern: organizations that fail at large-scale digital transformation do not fail because the technology doesn't work, they fail because the governance model cannot distribute decision rights fast enough to match the pace of platform development.
CVS faces a compounding constraint that most digital transformation case studies do not: every AI deployment operates inside a regulatory environment that treats data aggregation as a compliance risk rather than a strategic asset. HIPAA information barriers between Aetna's claims data and CVS Pharmacy's dispensing data require governance architecture as sophisticated as the technology architecture itself. The leadership transition from Karen Lynch to David Joyner in October 2024, mid-transformation, introduced an additional continuity risk, platform transformations of this complexity are acutely sensitive to shifts in internal political capital and prioritization sequencing.
Business Impact: Data Signals Anchoring the CVS Case Study
The quantitative evidence for CVS's transformation trajectory concentrates in adoption scale and cost efficiency rather than immediate margin expansion, consistent with a platform investment cycle. CVS now engages 185 million consumers annually across all touchpoints, with 60 million active digital customers as of January 2025. The platform processes 2.3 billion pharmacy claims annually, generating a transactional data foundation no digital health startup can replicate. Among CVS Specialty patients, 97% of active patients prefer digital two-way messaging with their CareTeam over traditional phone-based communication, a behavioral signal that validates the digital engagement thesis at the population level where it matters most commercially.
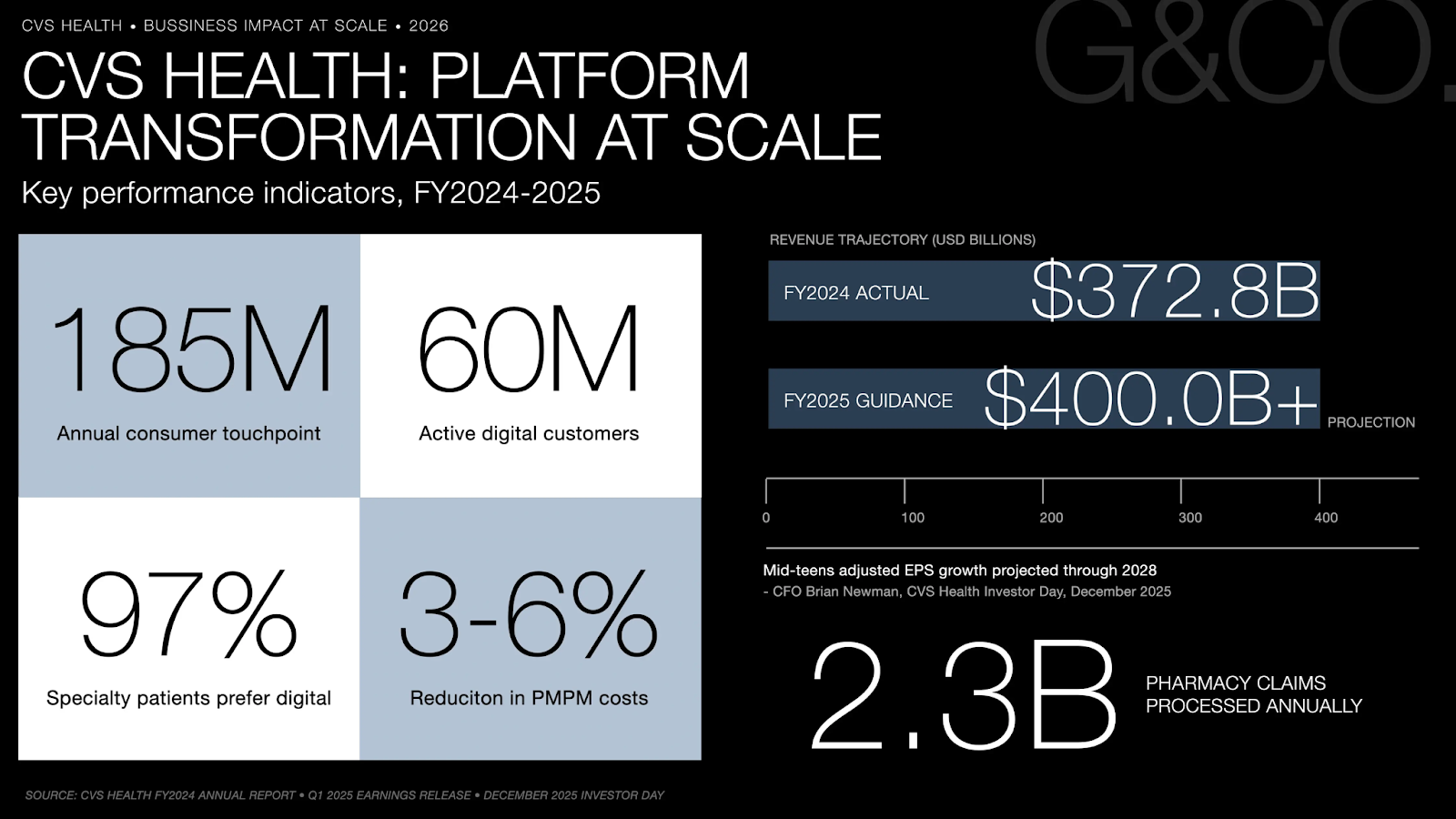
The financial trajectory supports the platform investment thesis. FY2024 revenue of $372.8 billion, growing to a projected $400 billion or more in FY2025, is accompanied by CFO Brian Newman's commitment to mid-teens adjusted EPS growth through 2028. The most structurally significant data signal, however, is the 3–6% decrease in per-member-per-month medical costs observed across integrated Aetna and Caremark members over three years. That metric is the proof-of-concept for the entire integration thesis, it demonstrates that data consolidation across the payer-PBM boundary produces measurable clinical and economic outcomes, not just UX improvements.
What This CVS Case Study Reveals at Scale
The repeatable enterprise pattern CVS's transformation crystallizes applies across any large-scale organization attempting to consolidate multiple acquired business units into a platform architecture: the consumer interface is the last thing built, not the first. The five years of infrastructure investment in data harmonization, API interoperability, and governance architecture are the precondition for the unified app, not its byproduct. Organizations that attempt to reverse this sequence, launching integrated consumer experiences before the underlying data layer is coherent, produce what the customer journey case study literature terms "facade integration", a unified front end masking a fragmented back end that eventually collapses under operational load.
CVS's scale also reveals a second pattern: the commercialization of internal infrastructure as an external product is only available to organizations that have fully solved the integration problem internally first. The "Engagement as a Service" ambition, selling the unified engagement platform to external employers and payers, is only credible because CVS is stress-testing it on 185 million of its own consumers. This mirrors the trajectory of Amazon Web Services, which commercialized internal infrastructure after proving it at internal scale. For enterprise leaders evaluating platform investment decisions, CVS's architecture decisions in 2023–2025 will likely serve as the template for regulated-industry platform consolidation for the next decade.
Strategic Reframe: This Is Not a Healthcare Story
The industry consensus frames CVS's transformation as a healthcare digitization story, an incumbent retailer-pharmacy-insurer adapting to digital-native consumer expectations. That framing underestimates the strategic logic. CVS is not digitizing healthcare. It is constructing a behavioral data platform that happens to be distributed through healthcare infrastructure. The distinction is consequential: a digitized healthcare company competes on care quality and cost efficiency, a behavioral data platform competes on data exclusivity, ecosystem lock-in, and the marginal cost of adding the next consumer or employer client to an already-amortized infrastructure.
The organizations that should feel most structurally threatened by CVS's transformation are not other pharmacy chains or health insurers. They are the health technology intermediaries, point solutions, digital therapeutics platforms, and patient engagement vendors, whose value proposition depends on CVS's data remaining siloed. Every integration milestone CVS achieves eliminates a category of vendor that was previously necessary. This is what makes the organizational challenge so strategically loaded: the faster CVS dissolves its internal silos, the faster it renders external dependencies obsolete, and the more defensible its platform position becomes.
Executive Takeaways
- Organizations that have grown through acquisition carry a structural data debt that compounds annually, CVS's transformation timeline reflects the true cost of resolving seven years of post-merger data fragmentation, not the cost of building new technology.
- Platform strategies in regulated industries require a governance architecture that evolves at the same velocity as the technology architecture, treating compliance as a deployment gate rather than a design input that consistently stalls platform investment cycles.
- The "Engagement as a Service" commercialization model is only available to enterprises that have achieved genuine internal integration first, attempting to sell external platform access before solving internal coherence exposes architectural incompleteness to the most sophisticated customers.
- Leadership transitions mid-transformation redistribute internal political capital in ways that can stall platform investment cycles precisely when momentum is most critical to sustaining organizational commitment.
- The consumer interface in a platform strategy is a data collection mechanism as much as an experience layer, enterprises that design digital consumer touchpoints without explicit data architecture intent build engagement infrastructure that cannot be monetized.
Why This Matters Now
The structural conditions that made CVS's transformation necessary, acquisition-driven scale, data fragmentation, margin pressure in core business units, and consumer expectations shaped by technology platforms outside healthcare, are not unique to healthcare. They describe the operating reality of every large-scale enterprise that grew through M&A in the 2010s and is now facing the compounding cost of deferred integration. The organizations executing this transition in 2025 and 2026 hold a material advantage: agentic AI healthcare infrastructure has reduced the cost and timeline of data harmonization significantly relative to what CVS faced in 2021. The window for platform consolidation has narrowed, not because the technology is more expensive, but because competitors who move first are establishing behavioral data moats that become structurally harder to close with each passing year.
Healthcare digital transformation at CVS's scale also reveals the limits of incremental digitization as a competitive strategy. The organizations that digitized individual processes, online prescription refills, telehealth booking, digital EOBs, are discovering that point-solution digital maturity does not compound into platform advantage. CVS's transformation demonstrates that the threshold between digitized enterprise and platform enterprise is not a continuum. It is a discrete architectural decision, made under earnings pressure, that requires leadership willing to absorb short-term performance costs for infrastructure that pays out on a five-year horizon.
Conclusion
CVS Health's transformation crystallizes a tension that defines enterprise strategy in the current period: the organizations best positioned to build platform advantage are the ones whose acquisition history created the most fragmented starting conditions. The Aetna acquisition that generated CVS's integration complexity is the same asset that makes the "Engagement as a Service" ambition credible; no digital health startup can replicate a 185-million-consumer behavioral data foundation built across payer, PBM, and pharmacy touchpoints simultaneously.
The enduring lesson is structural. CVS is not executing a digital transformation in the conventional sense, a technology upgrade overlaid on an existing operating model. It is executing an identity transformation, converting a holding company of distinct healthcare businesses into a single platform enterprise whose competitive moat is the data generated by their integration. The organizations that study this CVS case study most carefully are not healthcare companies. They are any enterprise sitting on fragmented post-acquisition data assets, wondering whether the cost of integration is justified by the strategic outcome. CVS's answer, playing out at $372.8 billion in annual revenue, is unambiguous.
Ready to explore a similar transformation?
Submit an inquiry to G & Co. on our contact page or click on the blue "Click to Contact Us" button on the bottom right corner of your screen for your convenience. We look forward to hearing from you.
Frequently Asked Questions
How did CVS Health execute its digital transformation strategy?
CVS Health consolidated three autonomous business units — Aetna, Caremark, and CVS Pharmacy — into a single AI-native engagement platform. Execution operated across four layers: a unified consumer app, Google Cloud agentic AI infrastructure, synthetic patient modeling via Agentic Twins, and clinician-facing AI tooling extending the engagement loop into care delivery.
Why did CVS Health pursue an omnichannel platform strategy rather than optimizing each business unit independently?
Independent optimization would have produced faster short-term gains but permanently foreclosed the integrated behavioral data layer underpinning CVS's long-term "Engagement as a Service" commercialization strategy. Leadership absorbed short-term earnings pressure to preserve platform architecture integrity — a trade-off that only makes strategic sense at CVS's scale of 185 million annual consumer touchpoints.
What is Agentic AI and how is CVS Health applying it in healthcare?
Agentic AI refers to AI systems that autonomously execute multi-step tasks without continuous human instruction. CVS deploys agentic AI across consumer navigation, synthetic patient modeling via Agentic Twins, and clinician support tools — making it one of the most comprehensive agentic AI healthcare deployments among U.S. payer-provider enterprises.
What were the measurable results of CVS Health's digital transformation?
CVS Health engages 185 million consumers annually with 60 million active digital customers. Integrated Aetna and Caremark members demonstrated a 3–6% decrease in per-member-per-month medical costs. CVS Specialty patients showed 97% preference for digital CareTeam communication. FY2024 revenue reached $372.8 billion with FY2025 guidance of $400 billion or more.
What can enterprise leaders learn from the CVS Health customer journey case study?
The primary lesson is sequencing: unified consumer experiences require coherent data infrastructure as their precondition, not their byproduct. Enterprises that launch integrated digital interfaces before solving back-end data fragmentation produce facade integration that cannot scale. CVS's five-year infrastructure investment before its January 2025 unified app launch is the architectural template for regulated-industry platform consolidation.






%20(1).png)




